-
posterior vitreous detachment (PVD) is a condition of the eye in which the vitreous membrane separates from the retina.
Broadly speaking, the condition is common for older adults and over 75% of those over the age of 65 develop it. Although less common among people in their 40s or 50s
Causes and risk factors
The vitreous is a gel which fills the eye behind the lens. Between it and the retina is the vitreous membrane. Over time the vitreous changes, shrinking and developing pockets of liquefaction. At some stage the vitreous membrane may peel away from the retina. This is usually a sudden event, but may also occur slowly over months.
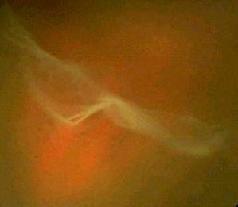
People with myopia (nearsightedness) greater than 6 diopters are at higher risk of PVD at all ages. Posterior vitreous detachment does not directly threaten vision. Even so, it is of increasing interest because the interaction between the vitreous body and the retina might play a decisive role in the development of major pathologic vitreoretinal conditions, such as an epiretinal membrane.
Symptoms
Flashes of light (photopsia)
A sudden dramatic increase in the number of floaters
A ring of floaters or hairs just to the temporal side of the central vision
As a posterior vitreous detachment proceeds, adherent vitreous membrane may pull on the retina. While there are no pain fibers in the retina, vitreous traction may stimulate the retina, with resultant flashes that can look like a perfect circle.
Complications
The risk of retinal detachment is greatest in the first 6 weeks following a vitreous detachment, but can occur over 3 months after the event.
The risk of retinal tears and detachment associated with vitreous detachment is higher in patients with myopic retinal degeneration, lattice degeneration, and a familial or personal history of previous retinal tears/detachment.
http://en.wikipedia.orgMore On Flashes Floaters and Spots
Location & Contact Details
© 2017 - 2024 Noel Templeton Optometrists



